

GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

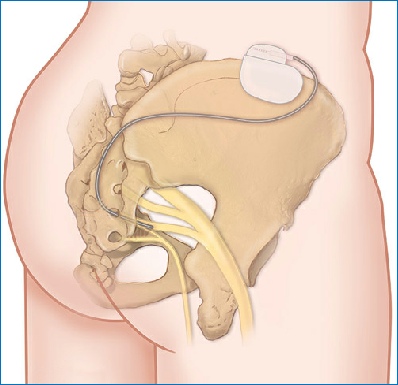 What is sacral nerve stimulation (SNS)?
What is sacral nerve stimulation (SNS)?
This is a procedure in which a small wire is used to stimulate the nerves coming from the sacrum (lower part of the backbone). The wire is connected to a small surgically implanted device (like a pacemaker) that generates the mild electrical impulses that stimulate the sacral nerve. This is mainly performed to help patients with bladder and bowel or faecal incontinence. Some doctors have also found that it may benefit other bowel problems such as constipation.
When is sacral nerve stimulation performed?
The most common reason for performing sacral nerve stimulation is to try and improve symptoms of both bladder and faecal incontinence. However, the information provided here is mainly focused on it’s use in patients with faecal or bowel incontinence. Patients with faecal incontinence most likely to benefit are those with intact muscles that do not work very well, though sometimes patients with damaged muscles benefit. It is becoming more widely used for some bowel problems and is occasionally used for patients with constipation.
What steps are required before being considered for sacral nerve stimulation?
Most patients having this operation will have had a colonoscopy or flexible sigmoidoscopy to assess the inner lining of their bowel. Specialised ultrasound and pressure studies are also usually performed to look the structure and function of the anus and anal muscles (anorectal physiology and endoanal ultrasound tests. It may also be necessary to assess if the bowel is working normally. A colonic transit study (to look at how quickly faeces passes through your bowel) and a defecating proctogram (to look at what happens to the inside of the rectum) when you open your bowels may also be necessary.
These tests are designed to look for damage to the sphincter muscle whilst ruling out other causes for your symptoms such as rectal prolapse or inflammation. If these other causes were found, then it might be necessary to consider different treatment options first, before sacral nerve stimulation.
What does the sacral nerve have to do with bowel control and faecal incontinence?
Nerves carry information to and from the brain about bowel evacuation and storage. When the communication system between the sacral nerves and the brain is not working, a person can have bowel control problems.
How does sacral nerve stimulation work?
It is not clear how sacral nerve stimulation works exactly. It certainly seems to stimulate the nerves that supply the muscles of the rectum and anus (back passage). However, this is only part of how it works and it is clear that there are other mechanisms at play that we do not fully understand. This may explain why some patients do not seem to get a benefit, despite appearing suitable on the basis of these investigations.
How is sacral nerve stimulation performed?
Because it is not possible to accurately predict which patients will benefit form sacral nerve stimulation, it is helpful to try out the stimulation for 2-
Temporary Sacral Nerve Stimulation
Patients who are considered likely to benefit from sacral nerve stimulation are first given a temporary or test wire. This is inserted with you awake after numbing the skin over the lower spine just above the buttocks. It usually takes about 30 minutes to insert these temporary wires. The other end of the wire is attached to a little stimulator (battery box) like an iPod which is worn on the belt.
The wire and stimulator connectors are all covered up with dressings. It is important not to bath or shower during the temporary test period as it is important that the dressings, the wire and stimulator stay dry and do not get dislodged. You will be shown how to disconnect the wire from the stimulator and we would recommend that you do this when driving.
This test period usually lasts two to three weeks and then the temporary wire is removed. Removal of the wire is straightforward and does not even require a local anaesthetic.
You will be given a diary to fill in so that your surgeon can assess how beneficial the temporary stimulator has been. About three quarters of patients improve with the temporary wire and are then offered a permanent implant
Permanent Sacral Nerve Stimulation
If the test which is performed with the temporary wire and stimulator is successful, then you can be considered for a permanent wire and stimulator.
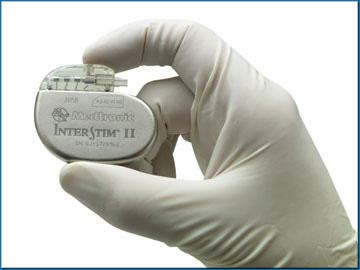
The permanent stimulator is inserted under a general anaesthetic. As for the temporary stimulator, a wire is inserted, but rather than come out through the skin to attach to the temporary box, it is tunnelled under the skin and attached to a small permanent stimulator buried in the fat of the buttock. The stimulator is the size of a small matchbox. At the end of this procedure, there are no visible wires or stimulators visible from the outside. You will usually be allowed home on the same day, from hospital.
What happens after insertion of the permanent implant?
When you are discharged, you will be given full instructions as well as contact details if you have any questions. You will be supplied with a wireless handset that communicates with the implanted stimulator, enabling you to turn it on and off and change the settings.
When the wounds have healed, you can shower and bath as usual. You can drive with the permanent implant as usual. Your doctor will keep you under regular review to ensure that you are continuing to benefit from the stimulator. Adjustments to the stimulator are often required to get the maximum benefit.
Are there any potential problems with sacral nerve stimulation?
Side effects may include, pain, skin irritation, infection, device problems and movement of the wires (leads) that connect between the stimulator and the sacral nerve.
Some patients complain of back or leg pain after placement of the permanent stimulator. If you get back pain, you should try turning off the stimulator for a couple of days. If the pain persists despite turning off the stimulator, it is unlikely to be due to the stimulator and you should consult your GP in the first instance. If the pain stops when the stimulator is turned off, then you need to get in contact with you specialist and it may be necessary to make adjustments to the stimulator.
How successful is sacral nerve stimulation in curing faecal incontinence?
Sacral nerve stimulation may reduce bowel symptoms for many people who suffer faecal incontinence, including the leakage of gas, liquid, or solid stool. Sacral nerve stimulation is reversible and can be discontinued at any time.
Although different centres have different results, the National Institute for Clinical Excellence (NICE) have published guidance on sacral nerve stimulation. Around 70-
In patients who have successful test and then go on to have permanent stimulator inserted, complete continence is achieved in 40-
How long does the battery in the permanent stimulator last?
It is variable, depending on the settings that are necessary to get the best effect. However, most patients will find that the stimulator works for at least 5 years before it has to be replaced.
Do insurance companies cover the cost of sacral nerve stimulation?
Many (but not all) of the main insurance companies in the UK will now pay for implantation of a sacral nerve stimulator. However, they may have specific criteria before they will fund the procedure, so it is important to check with them first.
Can I undergo sacral nerve stimulation in Glasgow Colorectal Centre?
Unfortunately, we are not currently able to offer Sacral Nerve Stimulation at present.
Sacral Nerve Stimulation (SNS) for Faecal Incontinence
Indication, mode of action and information about the procedure
This is a relatively new technique that can help restore continence in patients with bowel - faecal incontinence. It may also help with other bowel problems including constipation. With sacral nerve stimulation, a small implantable device is surgically placed to stimulate the sacral nerve with mild electrical impulses. The sacral nerve helps to control the bowel and muscles related to bowel function.

If you have any questions about sacral nerve stimulation or faecal incontinence, your own GP is often the best first port of call.
If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.