GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

What is rectal prolapse?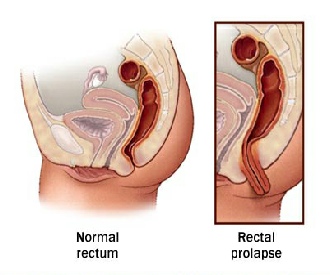
Rectal prolapse is a condition in which the rectum (the lower end of the colon, located just above the anus) becomes stretched out and protrudes out of the anus. The prolapse may comprise only of the inner lining of the rectum (rectal mucosa) and is called a ‘rectal mucosal prolapse’. This is similar to prolapsing haemorrhoids.
If the whole thickness of the rectal/bowel wall (both the inner mucosa and the outer muscle tube) has prolapsed, it is called a full thickness rectal prolapse or a complete rectal prolapse. On occasion, the prolapse may occur internally within the rectum (the rectum collapses inside itself). In this situation, no obvious prolapse may be seen coming out through the anus. This condition called an internal intussusception. Because there may be no obvious external prolapse, it is more difficult to diagnose and may require specialist x-
Rectal prolapse is often associated with weakness of the anal sphincter muscle, resulting in leakage of stool or mucus. Although a prolapsed bowel may occur in both sexes, it is much more common in women. It is also more common in the elderly and but occasionally may occur in young children.
Why does rectal prolapse occur?
Several factors may contribute to the development of rectal prolapse. Risk factors include the following
- Chronic constipation. It may come from a lifelong habit of straining to have bowel movements
- Excessive straining. Conditions such as prostatic hypertrophy, pregnancy, severe or chronic cough may predispose to rectal prolapse
- Weak pelvic floor which may follow childbirth or previous surgery.
- Genetic predisposition: In children, rectal prolapse may occur in association with cystic fibrosis, Ehlers-
Danlos syndrome and Hirschsprung’s disease - Old age: It seems to be a part of the aging process in many patients who experience stretching of the ligaments that support the rectum inside the pelvis as well as weakening of the anal sphincter muscle.
- Pelvic floor dysfunction, in association with urinary incontinence and pelvic organ prolapse as well.
- Neurological problems, such as spinal cord transection, spinal cord disease or multiple sclerosis may predispose to a prolapsed bowel.
In most cases, however, no single cause is identified.
Is rectal prolapse the same as prolapsed haemorrhoids?
Some of the symptoms may be the same: bleeding and/or tissue that protrudes from the rectum. Rectal prolapse, however, involves a segment of the bowel located higher up within the body, while haemorrhoids develop near the anal opening.
What are the symptoms of rectal prolapse?
The most obvious symptom of rectal prolapse is a lump or swelling coming out of the anus. Initially, this may only occur after a bowel movement. However, as the condition develops it may also happen when coughing or even when standing up.
With internal intussusception rectal prolapse, no lump or swelling comes through your anus. However, patients complain of a feeling of not having completely emptied their bowels, and many patients correctly describe actually feeling something sitting inside the rectum/anus.
With an external prolapse, it may be possible to push the prolapsed bowel back in. However, it may become difficult and as soon as it is pushed back in, it may protrude out again. Occasionally, it may not be possible to push it back in at all (termed ‘reduce the prolapse’).
Many patients with a rectal prolapse also notice that they have less than perfect control of their bowel movements. They may soil their underwear or have a slimy discharge from the rectum. These symptoms can make it difficult to maintain good hygiene. Occasional, bleeding may occur from the rectum and discomfort in the area.
How is rectal prolapse diagnosed?
A doctor can often diagnose this condition with a careful history and a complete anorectal examination. To demonstrate the prolapse, patients may be asked to sit on a commode and “strain” as if having a bowel movement.
Occasionally, a rectal prolapse may be "hidden" or internal, making the diagnosis more difficult. In this situation, an x-
Anorectal manometry and an endoanal ultrasound may also be used to evaluate the function of the muscles around the rectum as they relate to having a bowel movement. These tests are especially relevant if the rectal prolapse is associated with poor control (faecal incontinence).
If rectal bleeding or a change in bowel function occurs in association with the rectal prolapse, a telescope assessment of the colon may be necessary. This is called a flexible sigmoidoscopy (examination of the lower 1/3 of the rectum and colon) or a colonoscopy (the entire colon and rectum is examined)
How is rectal prolapse treated?
In the early stages, a minor rectal mucosal may respond to relief of constipation and straining by taking plenty of fruit and vegetables and other foods that contain fibre. Bulking laxatives, such as Fybogel may also help with bowel function.
In children, rectal prolapse usually gets better without any specific treatment. However, as with adults, it is important to avoid straining and parents or a child with rectal prolapse will be advised to ensure their child has plenty of fruit, vegetables and water in their diet, as well as foods that contain fibre.
Although constipation and straining may contribute to the development of a rectal prolapse, simply correcting these problems are unlikely to fix a full thickness rectal prolapse once it has developed. There are many different ways to surgically correct rectal prolapse.
Ultimately, an operation may be required. This may be performed via the abdomen or directly on the prolapse at the anus. The decision to recommend either abdominal or rectal surgery is based on a number of factors including age, physical condition, extent of prolapse, and the results of various tests.
An abdominal repair (rectopexy) aims to lift the rectum up and fix it so that it cannot prolapse out through the anus again. For many patients, this can be performed laparoscopically (keyhole repair of the prolapsed bowel). The repair is often reinforced with mesh to get the best long-
Rectal surgery may need to be performed in frail patients who are not suitable or not fit enough for an abdominal rectopexy. The most commonly performed rectal operation in this situation is called a DeLorme’s procedure. This is performed at the anus and may even be performed under spinal anaesthetic rather than a general anaesthetic.
How successful is treatment?
A great majority of patients are completely relieved of symptoms, or are significantly helped by the appropriate procedure. Success depends on many factors, including the status of a patient's anal sphincter muscle before surgery, whether the prolapse is internal or external and the overall health and fitness of the patient.
If the anal sphincter muscles have been weakened, either because of the rectal prolapse or for some other reason, they have the potential to regain strength after the rectal prolapse has been corrected. It may take up to a year to determine the ultimate impact of the surgery on bowel function.
Chronic constipation and straining after surgical correction should be avoided. Newer operations and particularly laparoscopic procedures are usually associated with a faster recovery. In particular, the operation named Laparoscopic Ventral Mesh Rectopexy (LVMR) appears to produce very good long-

If you have any questions about rectal prolapse or other colorectal issues, your own GP is often the best first port of call.
If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.
Rectal Prolapse
Symptoms, causes and treatment of rectal prolapse