GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

Anal Cancer
Symptoms, diagnosis and treatment of anal cancer
 What is the anus?
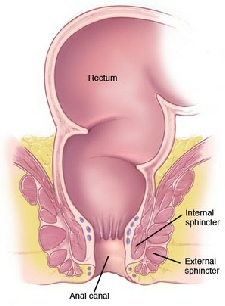
What is the anus?
The anus is the name for the muscular opening at the very end of the large bowel. It is controlled by a ring of muscle called a sphincter that opens and closes to control bowel movements. The area that connects the anus to the rectum is called the anal canal and is around 3–4 cm (1–1½in) long.
How common is anal cancer?
Cancer of the anus is rare. Around 1,000 people are diagnosed with anal cancer each year in the UK. The most common type of anal cancer is squamous cell carcinoma. Other rarer types are basal cell carcinoma, adenocarcinoma and melanoma. Early diagnosis and treatment is important to give the best chance of cure.
What causes anal cancer?
Anal cancer is slightly more common in women than in men. Many factors can increase your risk of developing anal cancer. These include:
- Human papilloma virus (HPV). Anal cancer is more likely to develop in people who’ve had a viral infection called the human papilloma virus (HPV). The risk of having HPV increases with the number of sexual partners you have.
- Sexual activity. People who have anal intercourse are more likely to develop anal cancer. This may be because they are more likely to have anal HPV. However, anal cancer can also develop in people who haven’t had anal intercourse or HPV.
- Lowered immunity. The immune system is part of the body's defence against infections and illnesses like cancer. Anal cancer is more common in people who have a lowered immunity, such as people taking medicines to suppress their immune system after an organ transplant or people with conditions such as HIV.
- Smoking. Smoking tobacco increases the risk of developing anal cancer. We have more information about stopping smoking.
Although these factors can increase a person’s risk of anal cancer, many people will not have these risk factors and the cause of their cancer remains unknown.
What are the symptoms of anal cancer?
The most common symptoms of anal cancer include:
- bleeding from the anus
- pain, discomfort and itching around the anus
- small lumps around the anus which may be confused with piles (haemorrhoids)
- difficulty controlling your bowels (faecal incontinence)
- discharge of a jelly-
like substance from the anus (mucus) - ulcers around the anus that can spread to the skin of the buttocks.
How is anal cancer is diagnosed?
If you are concerned about any symptoms, the best first step is to see you GP who will examine you and refer you to a colorectal specialist. At the hospital, the specialist will examine you and ask about your general health and any previous medical problems. They will do some tests before they can make a firm diagnosis of anal cancer.
Rectal examination
This is also sometimes known as a PR examination. A doctor examines your back passage with a gloved finger. Women may also have an internal examination of their vagina, as the vaginal wall is very close to the anal canal.
Biopsy
The doctor will put a thin tube into your back passage to examine the anal canal and rectum. This is called a proctoscopy. A small sample of tissue is taken from the tumour to be examined under a microscope (biopsy). This can be done under local or general anaesthetic. Sometimes a biopsy can be taken without needing to use a proctoscope.
If the tests show that you have anal cancer, you will need further tests to find out more about the position of the cancer and to see if it has begun to spread.
CT (computerised tomography) scan
A CT scan takes a series of x-
You may be given a drink or injection of a dye that allows particular areas to be seen more clearly. For a few minutes, this may make you feel hot all over. If you are allergic to iodine or have asthma you could have a more serious reaction to the injection, so it’s important to let your doctor know beforehand.
MRI (magnetic resonance imaging) scan
This test is similar to a CT scan but uses magnetism, instead of x-
Before having the scan, you’ll be asked to remove any metal belongings, including jewellery. Some people are given an injection of dye into a vein in the arm. This is called a contrast medium and can help the images from the scan show up more clearly. During the test you will be asked to lie very still on a couch inside a long cylinder (tube) for about 30 minutes. It’s painless but can be slightly uncomfortable, and some people feel a bit claustrophobic during the scan. It’s also noisy, but you’ll be given earplugs or headphones. You'll be able to hear, and speak to, the person operating the scanner.
PET-CT scan
This is a combination of a PET scan, which uses low-
Endoanal ultrasound scan
This uses sound waves to form a picture. A small probe that produces sound waves is passed into the back passage (rectum). This scan can show the size and extent of the tumour.The test is painless and takes about 30 minutes.
What are the stages of anal cancer?
The stage of a cancer is a term used to describe its size and whether it has spread beyond its original site. Knowing the particular type and stage of the cancer helps the doctors to decide on the most appropriate treatment.
Cancer can spread in the body, either in the bloodstream or through the lymphatic system. The lymphatic system is part of the body’s defence against infection and disease. It is made up of a network of lymph nodes connected by fine ducts containing lymph fluid. Your doctors will usually check the nearby lymph nodes when staging your cancer.
Stage 1
The cancer only affects the anus and is smaller than 2 cm (¾in) in size. It has not begun to spread into the sphincter muscle.
Stage 2
The cancer is bigger than 2 cm (¾in) in size, but hasn't spread into nearby lymph nodes or to other parts of the body.
Stage 3A
The cancer has spread to the lymph nodes near the rectum, or to nearby organs such as the bladder or vagina.
Stage 3B
The cancer has spread to lymph nodes in the groin and pelvis, or to lymph nodes close to the anus, as well as nearby organs such as the bladder or vagina.
Stage 4
The cancer has spread to lymph nodes in the abdomen or to other parts of the body, such as the liver.
A different staging system called the TNM staging system is sometimes used instead of the number system described above.
- T describes the size of the tumour and whether it has spread into nearby organs.
- N describes whether the cancer has spread to the lymph nodes.
- M describes whether the cancer has spread to another part of the body, such as the liver (secondary or metastatic cancer).
This system is more complex and can give more precise information about the tumour stage.
If the cancer comes back after initial treatment, it is known as recurrent cancer.
How is anal cancer treated?
The National Institute for Health and Clinical Excellence (NICE) recommends that people with an anal cancer are treated by a specialist team. These teams aren't available in all hospitals, so you may have to travel to another hospital for your treatment.
The main type of treatment for anal cancer is a combination of radiotherapy and chemotherapy. The two treatments are normally given at the same time (chemo-
Surgery may be used to treat small anal tumours or be used in combination with chemotherapy or radiotherapy for advanced anal cancer. Surgery may be used for small tumours. It can also be used if your treatment doesn't completely get rid of the cancer, or if there are signs that the cancer has returned. Sometimes it’s used if radiotherapy isn’t appropriate, for example if you’ve had radiotherapy to the area before. Occasionally it’s used to relieve symptoms before treatment with chemo-
Will I need a colostomy during my treatment for anal cancer?
The majority of patients treated for anal cancer will not need a colostomy. If the tumour does not respond completely to combination therapy, if it recurs after treatment, or if it is an unusual type, removal of the rectum and anus and creation of a colostomy may be necessary. This operation is known as an an abdomino-
What happens after treatment for anal cancer?
It's not unusual to have side effects for a time following treatment for anal cancer. These may include feeling bloated, having wind, diarrhoea and occasional incontinence. These side effects can be distressing but are usually temporary and improve over several months. Your doctor, nurse or dietitian will be able to give you advice about how to manage any side effects.
You will be followed up for between 5-
What do I do if I think I may have anal cancer?
Your first port of call is usually your own GP who will be able to assess you symptoms and decide if a referral to a colorectal specialist is appropriate.
Can I be seen at the Glasgow Colorectal Centre if I am worried that I might have anal cancer?
Yes. Glasgow Colorectal Centre Surgeons’ Richard Molloy and Ahmed Alani are happy to assess you and if necessary, perform a biopsy to confirm or exclude the diagnosis.
Summary of anal cancer information
Anal cancers are unusual tumours arising from the skin or mucosa of the anal canal. As with most cancers, early detection is associated with excellent survival. Most tumours are well treated with combination chemotherapy and radiotherapy. Recurrences may occur but often can be treated successfully. Follow the recommended screening examinations for anal and colorectal cancer and consult your doctor early if you develop any of the symptoms listed above.

If you have any questions about anal cancer or other colorectal issues, your own GP is often the best first port of call.
If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.