GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

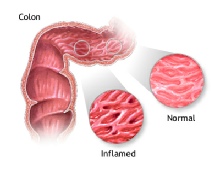
Who gets Inflammatory Bowel Disease (IBD)?
Anyone can get IBD, but it is most commonly diagnosed in adolescents and young adults between the ages of 15 and 25, but it can appear at any age. (Ten percent of those afflicted develop symptoms before the age of 18.). It is estimated that IBD affects about one person in every 250 in the UK. There are around 120,000 people with ulcerative colitis and 90,000 with Crohn's disease in the UK. IBD is more common in white people than in black people or those of Asian origin. The condition is most prevalent among Jewish people of European origin. IBD affects slightly more women than men.
Approximately 20 percent of patients have another family member with IBD, and families frequently share a similar pattern of disease.
IBD often imposes a significant impact on quality of life through ongoing symptoms, reduced ability to work, social stigma, bathroom access, difficulty with physical intimacy, and a restriction in career choices.
The unpredictable nature of these painful and debilitating digestive diseases create a significant burden on the community and the economy.
What causes ulcerative colitis and Crohn’s disease?
The exact causes of ulcerative colitis and Crohn’s disease are unclear. It is thought that several factors may play a part, such as:
- Genetics -
there is evidence that you are more likely to develop IBD if you have a close relative with the condition - Disruption to the immune system (the body’s defence against infection)
- Inflammation may be caused by the immune system attacking healthy tissue inside the digestive system whilst fighting off a virus or bacteria
- Environmental factors
- Autoimmune condition
What is the difference between ulcerative colitis and Crohn’s disease?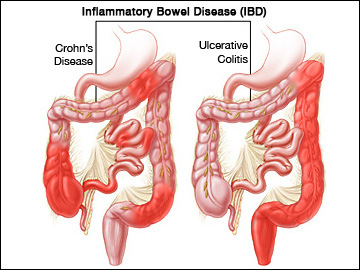
Ulcerative colitis affects only the rectum and colon and never affects the small intestine, whereas Crohn’s disease can cause inflammation anywhere along the digestive tract from the mouth, through stomach, small bowel and colon, rectum and anus.
Ulcerative also tends to cause inflammation only of the inner lining of the bowel (mucosa) whereas Crohn’s disease can also affect the muscle. Crohn’s disease may also cause areas of inflammation that are separate form each other whilst ulcerative colitis starts in the rectum and inflammation is continuous upstream from there.
What are the symptoms & complications of IBD?
Ulcerative colitis involves the inner lining of the colon, while Crohn's disease involves all layers of the intestine and can occur in both the small intestine and colon. Symptoms range from mild to severe and even life-
- Persistent diarrhoea abdominal pain or cramps
- Rectal bleeding
- Fever and weight loss
- Fatigue
- Joint, skin, or eye irritations o delayed growth in children
Crohn's disease and ulcerative colitis are unpredictable illnesses. Some patients recover after a single attack or are in remission for years. Others require frequent hospitalisations and surgery. Symptoms may vary in nature, frequency, and intensity. Without proper treatment, symptoms may worsen considerably and complications, such as abscesses, obstruction, malnutrition, and anaemia, are frequent.
Colon cancer may be a serious complication of long-
How is IBD treated?
There is currently no cure for ulcerative colitis or Crohn's disease. Treatment aims to relieve symptoms and prevent them from returning. Mild ulcerative colitis may not need treatment as symptoms can clear up after a few days. Medications currently available alleviate inflammation and reduce symptoms, but do not provide a cure or prevent long-
- Aminosalicylates (5-
ASA) (e.g. asacol) - Corticosteroids (e.g. prednisolone)
- Immunomodulators (e.g. azathioprine or 6-
MP) - Biologic therapies (e.g. infliximab)
- Antibiotics (e.g. metronidazole)
New treatments are being developed based on research of the immune system's role in the symptoms of IBD.
An estimated 20% of people with ulcerative colitis have severe symptoms that often don't respond to medication. In these cases, it may be necessary to surgically remove an inflamed section of the digestive system. Around 60-
What types of surgery are performed in IBD?
Surgery is sometimes recommended when medications can no longer control symptoms, when there are intestinal obstructions, or when other complications arise. An estimated two-
It is often possible to perform laparoscopic colorectal surgery for patients undergoing operation for IBD. This may be associated with a faster recovery and fewer complications.
Do emotional factors play any part in IBD?
IBD is not a psychosomatic illness-
Does diet have a role in treating or causing IBD?
There is no link between eating certain kinds of foods and IBD, but dietary modifications, especially during severe flare-
Where can I get more information on ulcerative colitis and Crohn’s Disease?
More detailed information on ulcerative colitis and Crohn’s disease is available on additional web-
UK patient orientated organisation. Provides useful information for patients with Crohn’s and colitis. Organisation had local branches and is also involved in fundraising
http://www.nhs.uk/conditions/Inflammatory-
Very good NHS website on Inflammatory Bowel Disease

If you have any further questions about Inflammatory Bowel Disease, Ulcerative Colitis or Crohn’s Disease, your own GP is often the best first port of call.
If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.
Inflammatory Bowel Disease
Causes, symptoms and treatment of inflammatory bowel disease
Inflammatory bowel disease (IBD) is a group of long-term conditions that cause inflammation of the gastrointestinal tract (gut). Crohn's disease & ulcerative colitis are the two commonest causes of IBD. Patients with IBD have inflammation of the intestine, leading to symptoms such as bloody diarrhoea, abdominal pain, weight loss and other problems. Medication does not cure IBD but can suppress inflammation and keep symptoms at bay. If medical therapy fails to control the symptoms, or if certain complications occur, surgery may be required.