GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

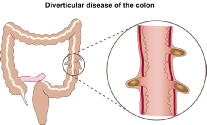
What is diverticular disease?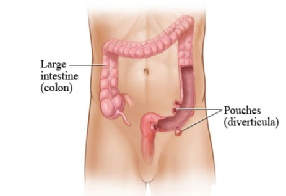
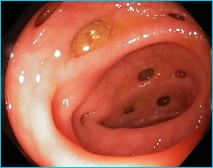
A diverticulum is the name given to a small pouch which bulges out from any hollow structure in the body. The plural of diverticulum is diverticula (used when there is more than one pouch). The terms diverticulosis or diverticular disease usually refer to diverticula bulging out of the colon.
Diverticula are common and associated with ageing. It is thought the pressure of hard stools (poo) passing through the large intestine that has become weakened with age causes the bulges to form.
What is the difference between diverticulitis and diverticular disease?
Medical words ending in ‘itis’ usually mean there is inflammation. The word diverticulitis describes the condition which occurs when diverticula become inflamed and painful. Diverticular disease (or diverticulosis disease) just means they are present.
How common is diverticular disease?
It is very common in western countries, especially with advancing age. It affects about 50 percent of Scottish adults by age 60 and nearly all by age 80. It is less common in Africa, possibly because of differences in diet (see diet below).
What causes diverticular disease?
The cause of diverticular disease and diverticulitis is not precisely known, but it is more common for people with a low fibre diet. Increased pressure within the bowel probably forces pouches of bowel lining through points of weakness in the muscle layers to form diverticula. Comparisons between different countries show that diverticular disease is more common in those countries with a western diet – high in animal protein and low in vegetable or cereal fibre. A low intake of fibre results in smaller volume of material passing through the colon, and in these circumstances the pressures produced inside the colon are higher. Thus, diverticular disease is thought to be one result of a low fibre diet.
Now that I have diverticular disease, will it ever go away?
Once diverticula have formed they are permanent, but that does not mean to say that they necessarily cause trouble. Most patients with diverticular disease have no symptoms at all.
Is diverticular disease associated with cancer?
There is no increased risk of cancer in diverticular disease. However since diverticular disease and bowel cancer may cause similar symptoms, your doctor may want to be entirely sure that he/she has excluded cancer by arranging an X-
What are the symptoms of diverticular disease?
Most patients with diverticular disease do not have any symptoms, and go through life unaware of the condition. Some patients experience:
- Change in bowel habit (either more constipated or more loose than usual)
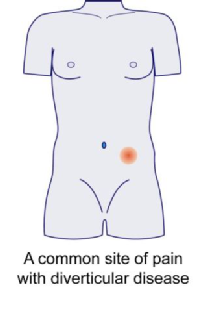
- Colicky discomfort, especially on the left side of the abdomen. 1 in 4 people with diverticula will experience symptoms such as abdominal pain.
- Distension of the abdomen
- Pain, which arises because the diverticula become inflamed (diverticulitis). This is less common
- Blood in the motions. If this occurs for the first time it is important to tell your doctor. This is rarely related to diverticular disease and other causes such as colon polyps and cancer should be excluded
How is uncomplicated diverticular disease treated?
A high-
- Wholemeal bread
- Brown rice
- Wholemeal pasta
- Plenty of fruit and vegetables
- Bran cereals
For many patients simply increasing vegetables in the diet will relieve their symptoms and return their bowel activity to normal. Fibre intake can be supplemented by adding coarse bran to food (e.g. to yogurt, soups, gravy, mashed potatoes, cereals etc). The doctor may prescribe dried fibre bulking agents:
- Ispagula husk – Fybogel, Regulan, Isogel, Metamucil, Vi-
Siblin - Sterculia – Normacol
- Methycellulose – Celevac, Cellucon, Cologel
These are other sources of fibre – often of natural origin (e.g. seed husks).
A few patients who still experience colicky pain and distension need treatment with drugs called antispasmodics or peppermint oil. These reduce the spasm in the colon which is often the cause of these symptoms.
Diverticulitis requires different management. Mild cases may be managed with oral antibiotics, dietary restrictions and possibly stool softeners. More severe cases require hospitalisation with intravenous antibiotics and dietary restraints. Most acute attacks can be relieved with such methods.
What complications may occur?
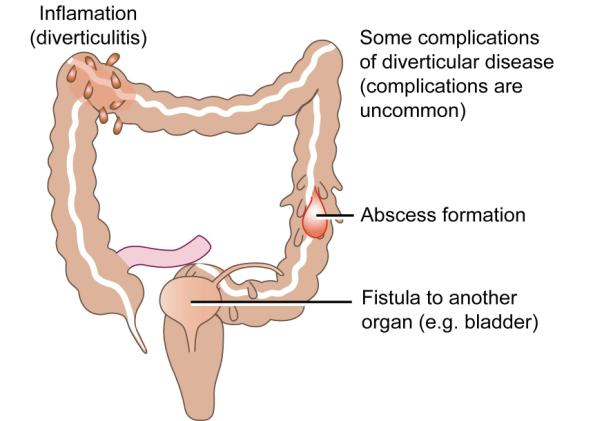
There are four main complications:
- Diverticulitis. This means inflammation of the diverticular disease. It is probably due to bacterial infection, and is usually treated by antibiotics. If the symptoms are severe, admission to hospital may be required and, rarely, a surgical operation.
- Perforation (bursting) of a diverticulum with acute peritonitis (generalised inflammation of the whole abdominal cavity). This is serious and requires urgent surgery.
- Abscess formation (a local collection of pus close to the colon due to a local perforation). The abscess may have to be drained surgically and the perforated piece of colon removed.
- Very rarely, formation of a fistula – perforation of a diverticulum into another structure, such as the bladder or vagina, and forming a connection. Odd symptoms, such as passing air in the urine or a discharge from the vagina, may develop. Surgery is the only treatment.
When is surgery necessary?
Surgery is reserved for patients with recurrent episodes of diverticulitis, complications or severe attacks when there's little or no response to medication. Surgery may also be required in individuals with a single episode of severe bleeding from diverticulosis or with recurrent episodes of bleeding.
In the past, surgery was recommended as a preventative measure for people who had two episodes of diverticulitis as a precaution to prevent complications. This is no longer the case as studies have found that in most cases risks of serious complications from surgery (estimated to be around one in a 100) usually outweigh the benefits. However, there are exceptions to this, such as: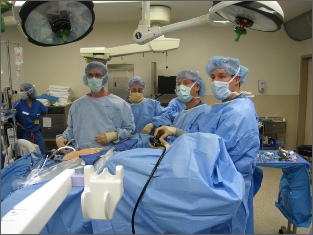
- History of serious complications arising from diverticulitis
- Symptoms of diverticular disease from a young age (it is thought the longer you live with diverticular disease, the greater your chances of having a serious complication)
- Weakened immune system or are more vulnerable to infections
- Recurrent bout of severe infection/inflammation (diverticulitis)
If surgery is being considered discuss both benefits and risks carefully with the doctor in charge of your care.
Colectomy
Surgery for diverticulitis involves removing the affected section of your large intestine. This is known as a colectomy. There are two ways this operation can be performed:
- An open colectomy, where the surgeon makes a large incision (cut) in your abdomen and removes a section of your large intestine
- A laparoscopic colectomy – a type of ‘keyhole surgery’ where the surgeon makes a number of small incisions in your abdomen and uses special instruments guided by a camera to remove a section of large intestine
Open colectomies and laparoscopic colectomies are thought equally effective in treating diverticulitis, and have a similar risk of complications. Laparoscopic colectomies have the advantage of having a faster recovery time, and cause less post-
Stoma surgery
In some cases, the surgeon may decide your large intestine needs to heal before it can be reattached, or that too much of your large intestine has been removed to make reattachment possible. In such cases, stoma surgery provides a way of removing waste materials from your body without using all of your large intestine. Stoma surgery involves the surgeon making a small hole in your abdomen known as a stoma. There are two ways this procedure can be carried out. These are explained below.
- An ileostomy, where a stoma is made in the right-
hand side of your abdomen (stomach). Your small intestine is separated from your large intestine and connected to the stoma, and the rest of the large intestine is sealed. You will need to wear a pouch connected to the stoma to collect waste material. - A colostomy, where a stoma is made in your lower abdomen and a section of your large intestine is removed and connected to the stoma. As with an ileostomy, you will need to wear a pouch to collect waste material.
In most cases the stoma will be temporary and can be removed once your large intestine has recovered from the surgery. This will usually take at least nine weeks. If a large section of your large intestine is affected by diverticulitis and needs to be removed, you may need a permanent ileostomy or colostomy.
What are the results of surgery?
In general terms, surgery is usually successful, although it does not achieve a complete cure in all cases. Following surgery, an estimated one in 12 people will have a recurrence of symptoms of diverticular disease and diverticulitis.
Can I undergo investigation and treatment for diverticular disease at the Glasgow Colorectal Centre?
Yes. Glasgow Colorectal Centre surgeons Richard Molloy and Ahmed Alani are experienced in the assessment and treatment of patients with diverticular disease.

If you have any further questions about diverticular disease or other colorectal issues, your own GP is often the best first port of call.
If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.
Diverticular Disease
Symptoms, causes and treatment of diverticular disease