GLASGOW COLORECTAL CENTRE
Scotland’s Best Private Colorectal Surgery & Colonoscopy Clinic
info@colorectalcentre.co.uk
If you have any questions, call Catherine on 0735 506 6597

© Glasgow Colorectal Centre. All Rights Reserved

 Book an Appointment
Book an Appointment
Any questions? Call Catherine on 0735 506 6597
Info@colorectalcentre.co.uk

Who should have a colonoscopy?
Colonoscopy may be recommended to adults 50 years of age or older who are found to have tiny traces of blood in stool samples submitted as part of the Bowel Screening Program. Patients with a family history of colon or rectal cancer may also need to consider having a colonoscopy, even if they do not have any bowel symptoms. Your doctor may also recommend a colonoscopy examination if you have had a change in bowel habit or you have noticed rectal bleeding. These symptoms indicate a possible problem in the colon or rectum. A colonoscopy may be necessary to:
- Check unexplained abdominal symptoms
- Check inflammatory bowel disease (colitis)
- Verify findings of polyps or tumours located with a barium enema exam
- Examine patients who test positive for blood in the stool (positive bowel screening test)
- Monitor patients with a personal or family history of colon polyps or cancer.
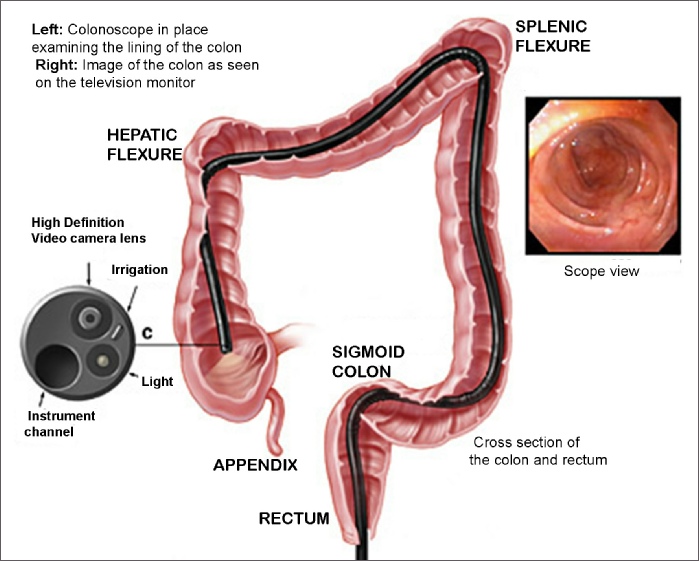
How is colonoscopy performed?
The bowel must first be thoroughly cleared of all residue before a colonoscopy. This is done one days before the exam with a preparation prescribed by your doctor. Many patients receive intravenous sedation, or “conscious sedation” for this procedure. This means that they may be a little drowsy but the aim is not to make them fully unconscious. The colonoscope is inserted into the rectum and is advanced to the portion of the colon where the small intestine joins the colon. During a complete examination of the bowel, your doctor may also remove polyps or take biopsies as necessary.
The entire procedure usually takes less than 30 minutes. Following the colonoscopy, there may be slight discomfort, which quickly improves with the expelling of wind. Most patients can resume their regular diet and activities the same day. If they have had sedation, they should not drive, operate machinery or sign any legal documents for the rest of the day.
What are the benefits of colonoscopy?
Colonoscopy is more accurate than an x-
What are the risks of colonoscopy?
Colonoscopy is generally a very safe procedure with complications occurring in less than 1% of patients. These risks include bleeding, a tear in the intestine, risks of the sedation and failure to either complete the examination or failure to detect a polyp or other pathology.
What are the reasons for an incomplete colonoscopy?
You might expect an experienced doctor who performs a lot of colonoscopy to to be able to complete the examination around 95% of the time. There are a number of reasons why it might not be possible to complete the examination. These include the following
- Patient was not able to take all the laxatives before the procedure so the bowel is not fully cleaned out
- It is not possible to pass the colonoscope through a narrowing or stricture in the bowel. Narrowed areas may be caused by cancer, diverticular disease, Crohn’s disease
- The bowel is very twisty or tortuous or very long which impedes progress.
What happens if it is not possible to perform a complete colonoscopy?
You doctor will discuss why it was not possible to complete the examination. Depending on the indication for the procedure and also taking into account how much of the colon was examined, they may recommend an additional test such as a CT pneumocolon (also known as a CT colonoscopy). Although this is a good second best examination in the event that it is not possible to complete the colonoscopy, it does suffer from the drawback in that if a problem is seen, it is not possible to obtain a biopsy or remove colonic polyps if these are identified.
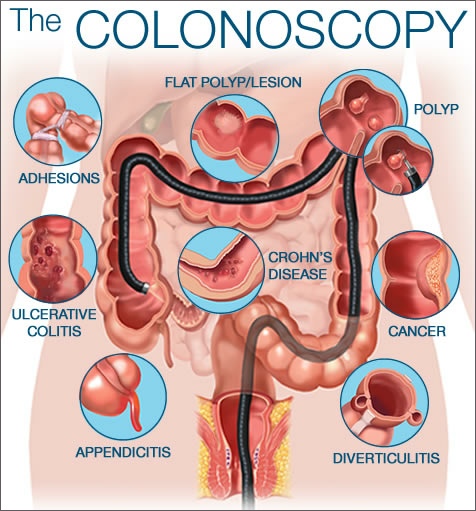
What sort of conditions can be diagnosed at colonoscopy?
Any diseases affecting the ling of the colon or even the terminal ileum (small bowel leading into the colon) can be diagnosed at colonoscopy. Most examinations are normal. However, some of the more commonly conditions that may be found at colonoscopy include the following
- Haemorrhoids
- Diverticular disease
- Colon and rectal polyps
- Inflammatory bowel disease such as ulcerative colitis, Crohn’s disease or proctitis
- Colon and rectal cancer
- Strictures or narrowed areas of the colon
Is it possible to have a Private Health colonoscopy at the Glasgow Colorectal Centre?
Our surgeons, Mr. Richard Molloy and Mr. Ahmed Alani perform colonoscopy as a routine part of their clinical practice. Both have colonoscopy completion rate of more than 95%. Our surgeons also perform colonoscopy as part of the NHS Colorectal Cancer Screening program. They are experienced at advanced & therapeutic colonoscopy including complex polypectomies, endoscopic mucosal resection (EMR) and dilatation (opening up) of colonic strictures etc.
The Glasgow Colorectal Centre is based at Ross Hall hospital. The hospital has recently opened a new state of the art dedicated endoscopy suite, with the very latest high definition Olympus colonoscopes. It has its own entrance/reception which directly lead into the patient rooms and the endoscopy suite.


If you have any questions about colonoscopy or other colorectal issues, your own GP is often the best first port of call. If appropriate, they will be able to arrange a referral to a colorectal specialist centre such as the Glasgow Colorectal Centre.
Colonoscopy
Indications, preparation & procedure information
Colonoscopy is a safe, effective method of examining the full lining of the colon and rectum, using a long, flexible, tubular instrument. It is used to diagnose colon and rectum problems and to perform biopsies and remove colon polyps (polypectomies). Most colonoscopies are performed as an outpatient, with minimal inconvenience and discomfort.